Why Blood Sugar Affects Your Vision
How Does Diabetes Affect My Eyes?
High blood sugar damages blood vessels throughout your body including the tiny, delicate vessels in your retina. This damage is called diabetic retinopathy, and it’s the most common cause of blindness in working-age adults.
Here’s what’s important: Diabetic eye disease is preventable and treatable when caught early. But it requires vigilance, from both you and your eye doctor.
What Is Diabetic Retinopathy?
Your retina is like the film in a camera, it captures the images you see. Diabetic retinopathy occurs when high blood sugar damages the blood vessels feeding your retina.
Early Stage (Non-Proliferative): Vessels weaken and bulge, small amounts of fluid leak, and there are usually no symptoms you can detect.
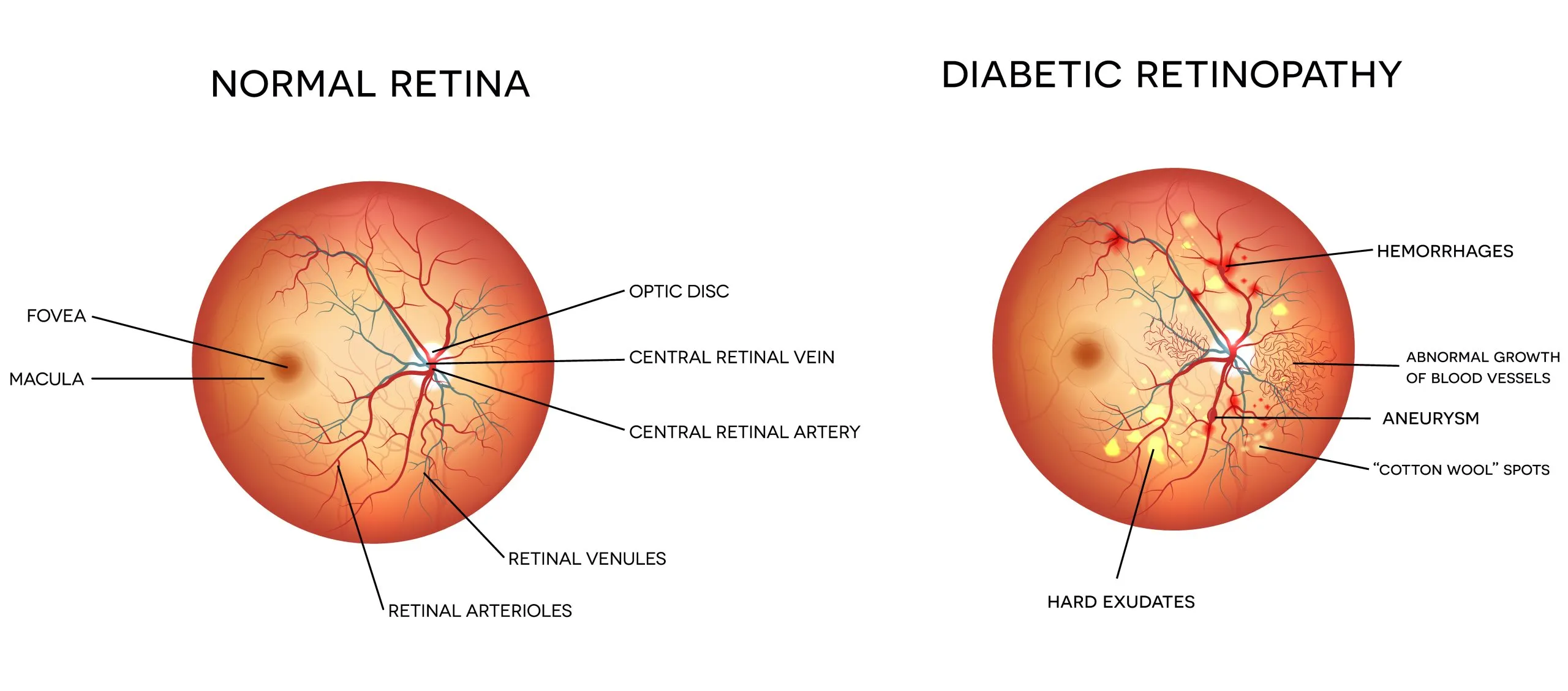
Advanced Stage (Proliferative): New, fragile blood vessels grow that bleed easily, can cause sudden vision loss, and scar tissue can form, pulling on the retina.
Will I Know If I Have It?
Not at first. That’s the dangerous part.
Early diabetic retinopathy has zero symptoms. No pain, no blurriness, no warning signs. By the time you notice vision changes, significant damage has often occurred.
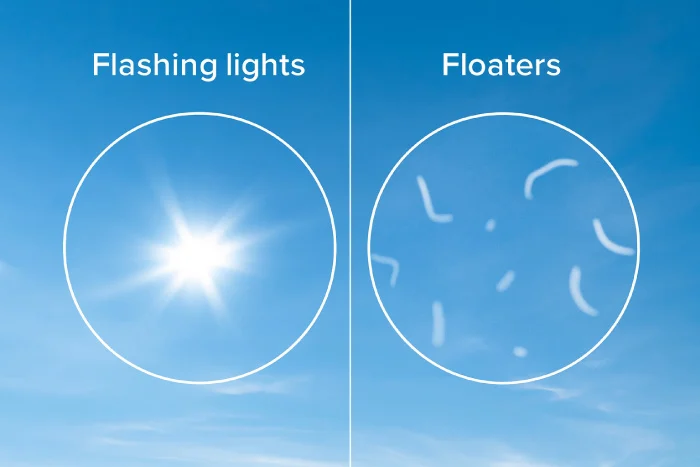
Later symptoms might include floaters (dark spots or strings in your vision), blurred or fluctuating vision, dark or empty areas in your vision, poor color vision, or vision loss.
Sudden vision loss is an emergency. Call your eye doctor immediately.
I Just Got Diagnosed with Diabetes. How Soon Should I Get My Eyes Checked?
Type 1 diabetes: Within 5 years of diagnosis
Type 2 diabetes: Immediately (you may have had diabetes for years before diagnosis)
Pregnant with diabetes: First trimester and monitored throughout pregnancy
After that: Annually, or more often if retinopathy is detected by your eye doctor.
What Else Can Diabetes Do to My Eyes?
Beyond retinopathy, diabetes increases risk for:
Diabetic macular edema: Swelling in the macula (center of retina) that blurs your central vision.
Glaucoma: Diabetes doubles your risk for this sight-threatening condition.
Cataracts: They develop earlier and progress faster in people with diabetes.
Double vision: Blood sugar affects nerves controlling eye movement.
Blurry vision: Blood sugar fluctuations cause temporary vision changes (this isn’t damage, it’s your lens swelling and shrinking).
How Long Does a Stye Last?
Your eye doctor does more than check if you need glasses. Here’s what to expect:
Step 1: Dilated eye exam: Drops widen your pupils so we can see your entire retina.
Step 2: Retinal photography: Documents any changes so we can track progression over time.
Step 3: OCT imaging: Shows detailed cross-sections, revealing swelling or fluid that’s invisible
to the naked eye.
Step 4: Pressure check: Screens for glaucoma, which diabetics are at higher risk for.
Step 5: Complete medical history: We’ll review your A1C levels, blood sugar control, and
medications.
The exam takes about 45-60 minutes. Your vision will be blurry for a few hours after dilation. Bring sunglasses and plan for someone else to drive.
Can Diabetic Retinopathy Be Treated?
Yes! Treatment options depend on severity:
For Early Stages: Blood sugar control (the single most important factor), blood pressure management, and regular monitoring every 3-12 months with your eye doctor.
For Advanced Stages: Laser treatment (seals leaking vessels and prevents new growth), anti-VEGF injections (reduces swelling and abnormal vessel growth), steroid injections (reduces inflammation and swelling), or vitrectomy surgery (removes blood or scar tissue in advanced cases).
What's the Single Most Important Thing I Can Do?
Control your blood sugar. Period.
Studies show that keeping your A1C below 7% dramatically reduces your risk of developing diabetic retinopathy, and slows progression if you already have it. Think of good blood sugar control as preventive treatment for your eyes.
Does Blood Pressure Matter Too?
Absolutely. High blood pressure compounds the damage diabetes does to your retinal blood vessels. Controlling both together gives you the best protection. Your eye doctor will work with your primary care physician to ensure you’re getting comprehensive care.
I Don't Have Symptoms. Do I Really Need Yearly Exams?
Yes, this is crucial.
Diabetic retinopathy can be treated and vision can be saved if caught early. But once significant vision loss occurs, it’s often permanent. Annual dilated exams with your eye doctor catch problems when they’re still treatable. Don’t wait until you notice symptoms.
Will My Vision Fluctuate Day to Day?
Possibly. When blood sugar runs high or low, your lens temporarily swells or shrinks. This causes blurry vision that comes and goes. It’s frustrating but not harmful.
Don’t rush to get new glasses when your blood sugar is uncontrolled. Wait until it’s stable for a few weeks, otherwise your new prescription will be wrong
I'm Pregnant and Have Diabetes. Is That Different?
Yes, pregnancy can accelerate diabetic retinopathy. You need an eye exam in your first trimester, follow-up exams each trimester, and a postpartum exam. Don’t skip these appointments. Your eye doctor will work closely with your OB-GYN and endocrinologist.
What Questions Should I Ask My Eye Doctor?
Do I have any signs of diabetic retinopathy? If yes, what stage am I in? How often do I need to be monitored? What’s my target A1C to protect my eyes? Are there other diabetes-related eye issues I should watch for?
The Bottom Line
Diabetes doesn’t have to steal your vision. Yes, it puts your eyes at risk, but you have tremendous control over that risk through blood sugar control, blood pressure management, dilated eye exams annually (or as recommended), not smoking, and reporting any vision changes immediately.
We’re your partner in this. Think of your annual diabetic eye exam not as “checking for problems,” but as actively protecting your sight.
Living with diabetes? Our diabetic eye exams include advanced imaging technology that detects problems before they affect your vision. Partner with us to protect your sight for years to come.